Signs Of Heart Failure In Cancer Patients
What is heart failure?
Your heart is a muscle that works 24/7 to pump oxygenated blood throughout your body. Some conditions can take a toll on the heart muscle, causing it to weaken or stiffen. When this happens, the heart pumps inefficiently. Heart failure exists when the heart can no longer pump enough blood to meet the body’s needs.
There are two types of heart failure:
- Right Sided Heart Failure
- Left Sided Heart Failure
Right Sided:
Right sided heart failure means your heart’s right ventricle is too weak to pump enough blood to the lungs. Blood builds up in your veins, vessels that carry blood from the body back to the heart.
Left Sided:
The left ventricle of the heart no longer pumps enough blood around the body. Blood builds up in the pulmonary veins. This cause shortness of breath, trouble breathing or coughing especially during physical activities.
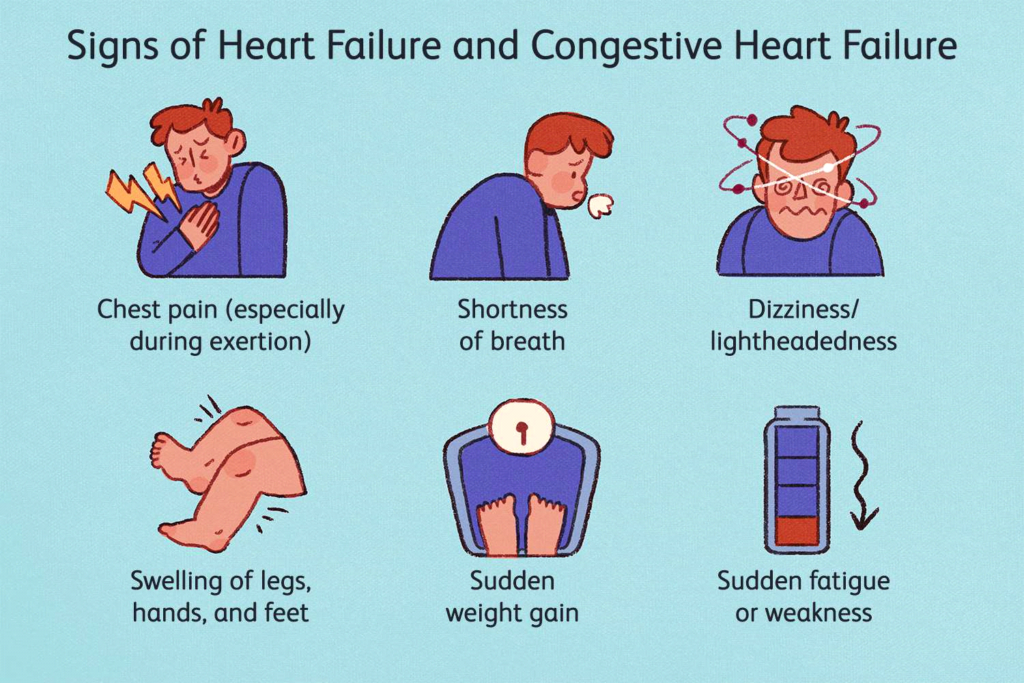
Heart Failure Symptoms:
Shortness of breath during physical activities or when laying down.
Fatigue
Weakness
Swelling in the legs, ankles and feet.
Rapid or irregular heartbeat
Wheezing
Swelling of the belly area
Very rapid weight gain from fluid buildup
Nausea and lack of appetite
Chest pain
Diagnosing Heart Failure:
- Blood tests: To check whether there’s anything in your blood that might indicate heart failure.
- ECG (electrocardigram): This records the electrical activity of your heart to check for problems.
- Echocardiogram: A type of ultrasound scan where sound waves are used to examine your heart.
- Breathing tests: You may be asked to blow into a tube to check whether a lung problem is contributing to your breathlessness.
- A chest X-ray: To check whether your heart’s bigger than it should be, whether there’s fluid in your lungs.
Signs Of Heart Failure In Cancer Patients
Cancer patients, particularly those undergoing certain types of cancer treatments, may be at risk of developing heart-related complications, including heart failure. Some cancer therapies, such as certain chemotherapy drugs and radiation therapy, can have cardiotoxic effects that impact the heart’s function. Here are some signs of heart failure that cancer patients should be aware of:
Shortness of Breath (Dyspnea):
Difficulty breathing or shortness of breath, especially during physical activity or while lying down, can be a sign of heart failure. It may be due to the heart’s reduced ability to pump blood effectively.
Fatigue and Weakness:
Persistent fatigue and weakness that are not relieved by rest may be indicative of heart failure. In the context of cancer treatment, this can be a sign of the heart’s struggle to meet the body’s demands.
Fluid Retention (Edema):
Swelling in the legs, ankles, abdomen, or other parts of the body may occur when the heart is not effectively pumping blood. Fluid retention is a common symptom of heart failure.
Rapid or Irregular Heartbeat:
Changes in heart rhythm, including a rapid or irregular heartbeat (arrhythmia), may be associated with heart failure. These changes can be felt as palpitations.
Coughing and Wheezing:
A persistent cough, especially one that produces pink or bloody sputum, may be a sign of fluid accumulation in the lungs, a condition known as pulmonary edema.
Reduced Exercise Tolerance:
A noticeable decrease in the ability to engage in physical activities or exercise may indicate compromised cardiac function.
Weight Gain:
Unexplained weight gain, often due to fluid retention, can be associated with heart failure.
It’s important for cancer patients to communicate openly with their healthcare team about any new or worsening symptoms, especially those related to heart health. Regular monitoring of cardiac function may be recommended for patients undergoing cancer treatments with known cardiotoxic effects.
Additionally, healthcare providers may perform baseline assessments of cardiovascular health before initiating cancer treatments that carry a risk of cardiotoxicity. This allows for early detection of any cardiac issues and the implementation of preventive measures or adjustments to the treatment plan.
Congestive Heart Failure:
Congestive heart failure is a serious condition in which the heart doesn’t pump blood as efficiently as it should. It means that the heart muscle has become less able to contract over time.
Prevention
- Stop smoking
- Eat in healthy ways
- Lose weight if you are over weight
Lifestyle:
Adopting a heart-healthy lifestyle can play a crucial role in preventing or managing congestive heart failure. Here are some lifestyle changes that may help:
Healthy Diet:
Heart-Healthy Foods: Choose a diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats. Limit saturated and trans fats, cholesterol, sodium, and added sugars.
Regular Exercise:
Aerobic Exercise: Engage in regular aerobic exercises, such as walking, swimming, or cycling, for at least 150 minutes per week. Exercise helps improve heart function and overall cardiovascular health.
Maintain a Healthy Weight:
Weight Management: Achieve and maintain a healthy weight to reduce the workload on the heart. Losing excess weight can improve heart function and decrease strain on the cardiovascular system.
Manage Blood Pressure:
Blood Pressure Control: Monitor and manage blood pressure within a healthy range. This may involve lifestyle changes, medication, or a combination of both.
Manage Cholesterol Levels:
Cholesterol Control: Keep cholesterol levels in check by adopting a heart-healthy diet, exercising regularly, and, if necessary, taking prescribed medications.
Limit Alcohol Intake:
Moderate Drinking: If you consume alcohol, do so in moderation. Excessive alcohol intake can contribute to heart failure.
Quit Smoking:
Smoking Cessation: Quit smoking if you are a smoker. Smoking is a major risk factor for heart disease and can worsen heart failure.
Manage Diabetes:
Blood Sugar Control: If you have diabetes, manage blood sugar levels through a combination of healthy eating, regular physical activity, and medication as prescribed by your healthcare provider.
Limit Sodium Intake:
Sodium Restriction: Reduce sodium intake by avoiding processed foods, using herbs and spices for flavor, and limiting added salt during cooking and at the table. Sodium restriction helps prevent fluid retention.
Regular Medical Check-Ups:
Monitoring and Management: Regularly monitor your health, attend follow-up appointments with your healthcare provider, and adhere to prescribed medications and treatment plans.
Stress Reduction: Practice stress-reducing techniques such as deep breathing, meditation, yoga, or hobbies to manage stress, which can impact heart health.
Limit Caffeine Intake:
Moderate Caffeine Consumption: While moderate caffeine intake is generally considered safe, excessive consumption may contribute to increased heart rate and blood pressure.